Insurers cut back GLP-1 coverage as demand soars: Found study
4.9 (637) · $ 23.99 · In stock

As demand surges for GLP-1 therapies, insurers are pulling back on coverage, according to new data from obesity care provider Found. | Sarah Jones Simmer, CEO of Found, said that the trends are likely the result of irresponsible prescribing for recreational reasons causing the pendulum to swing "all the way in the other direction," and it's leading to patients who have genuine medical need struggling to access these therapies.

3 Reasons ResMed's CEO Isn't Worried About Ozempic or Wegovy

Weight-loss drug Wegovy can be marketed for heart benefits after FDA label update
20% of Americans Would Change Jobs to Gain Ozempic, Wegovy Coverage

The Impact of GLP-1 Coverage and Spend on Pharmacy Benefits Costs - New
Ontario limiting access to Ozempic to conserve supply for those

New Classes Of Obesity Drugs Face Strong Headwinds From Insurers

As the market for new weight loss drugs soars, people with diabetes pay the price

Tsunami of exclusion': Patients face aftermath of GLP-1 cuts

As demand for Ozempic soars, Ontario puts limits on coverage under Ontario Drug Benefit Plan
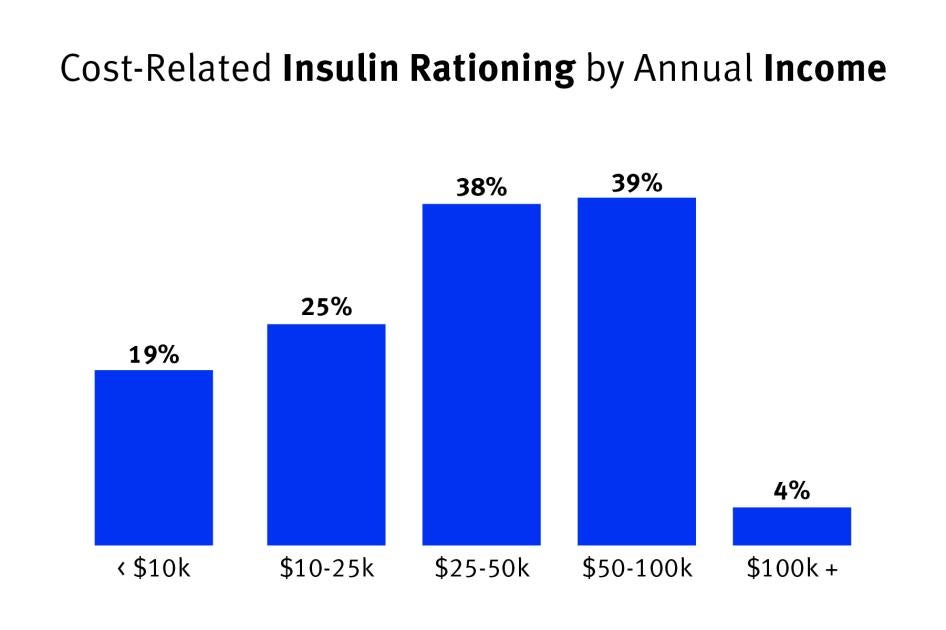
If I'm Out of Insulin, I'm Going to Die”: United States' Lack of Regulation Fuels Crisis of Unaffordable Insulin

The Doctor Prescribed an Obesity Drug. Her Insurer Called It 'Vanity.' - The New York Times